There is more and more evidence suggesting that ultrasound-guided musculoskeletal injections and interventions are more accurate and yield better results than blind or landmark-guided procedures. However, learning the proper techniques remains a barrier for many clinicians.
When Orthopedic Surgeon Dr. Alan Hirahara began using ultrasound in 2009 to guide his injections, he noticed his patients were experiencing significantly less pain during the procedures. Now a strong advocate for the use of ultrasound to guide injections, Dr. Hirahara has developed new techniques to make injections easier, more precise, and less painful for his patients.
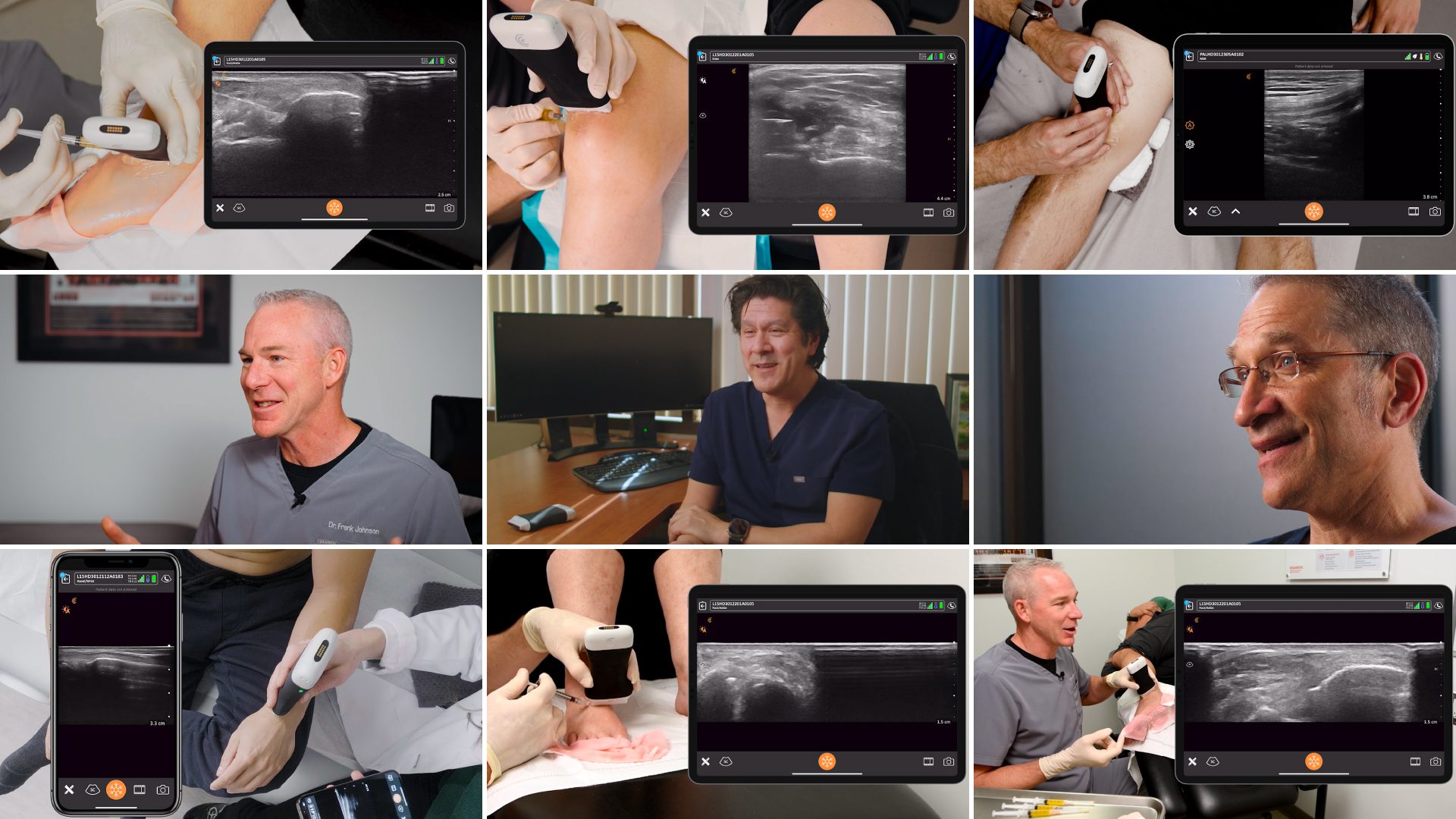
That’s why we’re working with Dr. Hirahara on a series of upcoming webinars during which he will share his techniques for performing ultrasound-guided MSK Injections. You’ll see numerous recorded procedures performed on a cadaver and live scanning with Clarius HD3.
The first of the webinar series, Expert Ultrasound Guidance for Accurate MSK Injections, Part 1: The Shoulder, is available to watch on-demand now. Read on for highlights and video snippets from the webinar on how to perfect your ultrasound scanner placement for the best visualization of your needle and target shoulder anatomy.
Musculoskeletal (MSK) Ultrasound
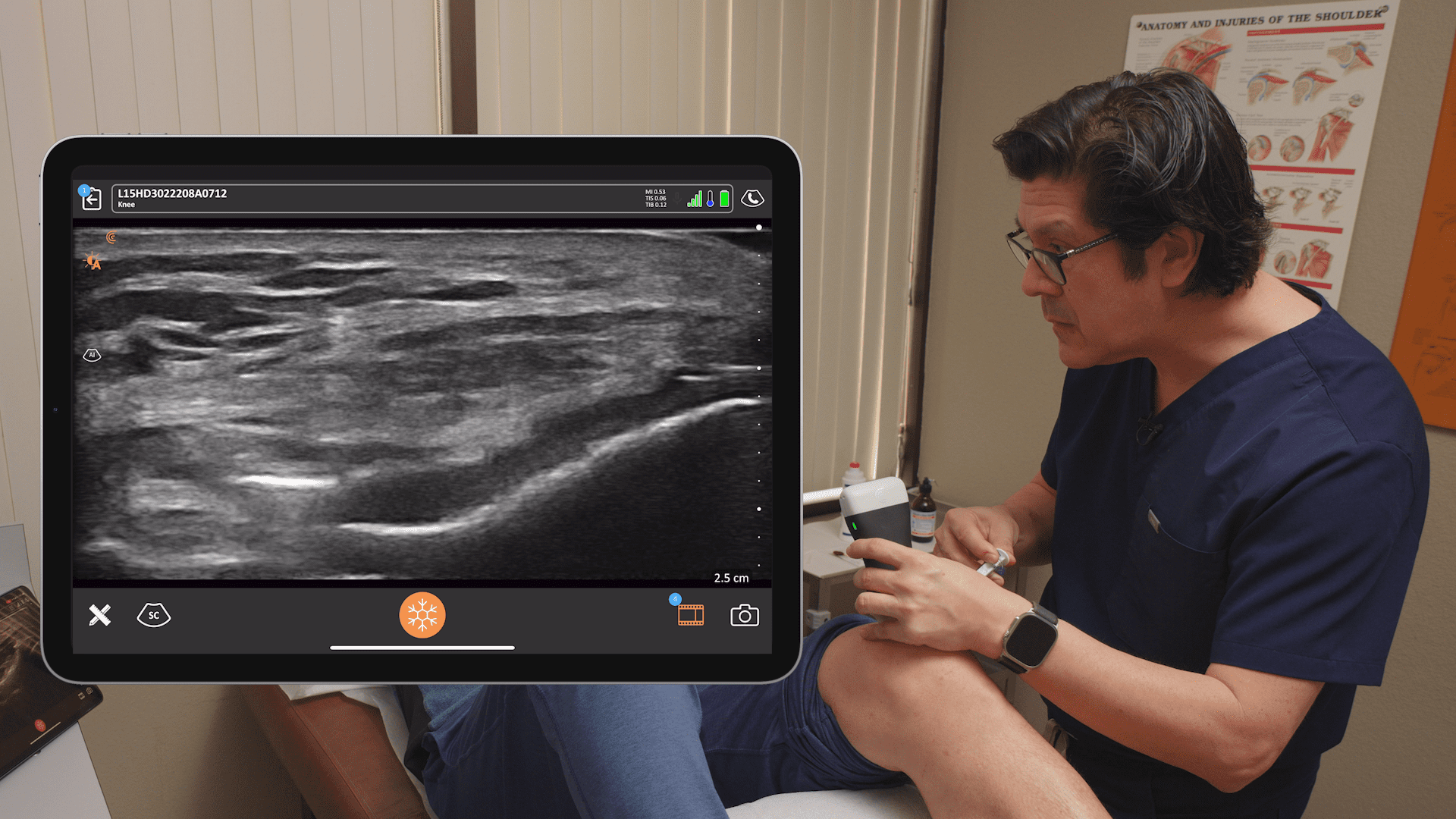
According to Dr. Hirahara, an understanding of how the ultrasound beam interacts with tissues in the body, particularly tendons, muscles, and joint spaces, is key to getting the best images. For optimal visualization, and to avoid an ultrasound artifact known as anisotropy, position the scanner so that the anatomy you’re interrogating is perpendicular to the sound beam.
Anisotropy is an important pitfall encountered with MSK imaging. If the tendon or muscle being imaged is not perpendicular to the sound beam, the appearance of the tendon may become more hypoechoic, and loss of detail can occur. A simple toggling or tilting of the scanner can help to overcome anisotropy.
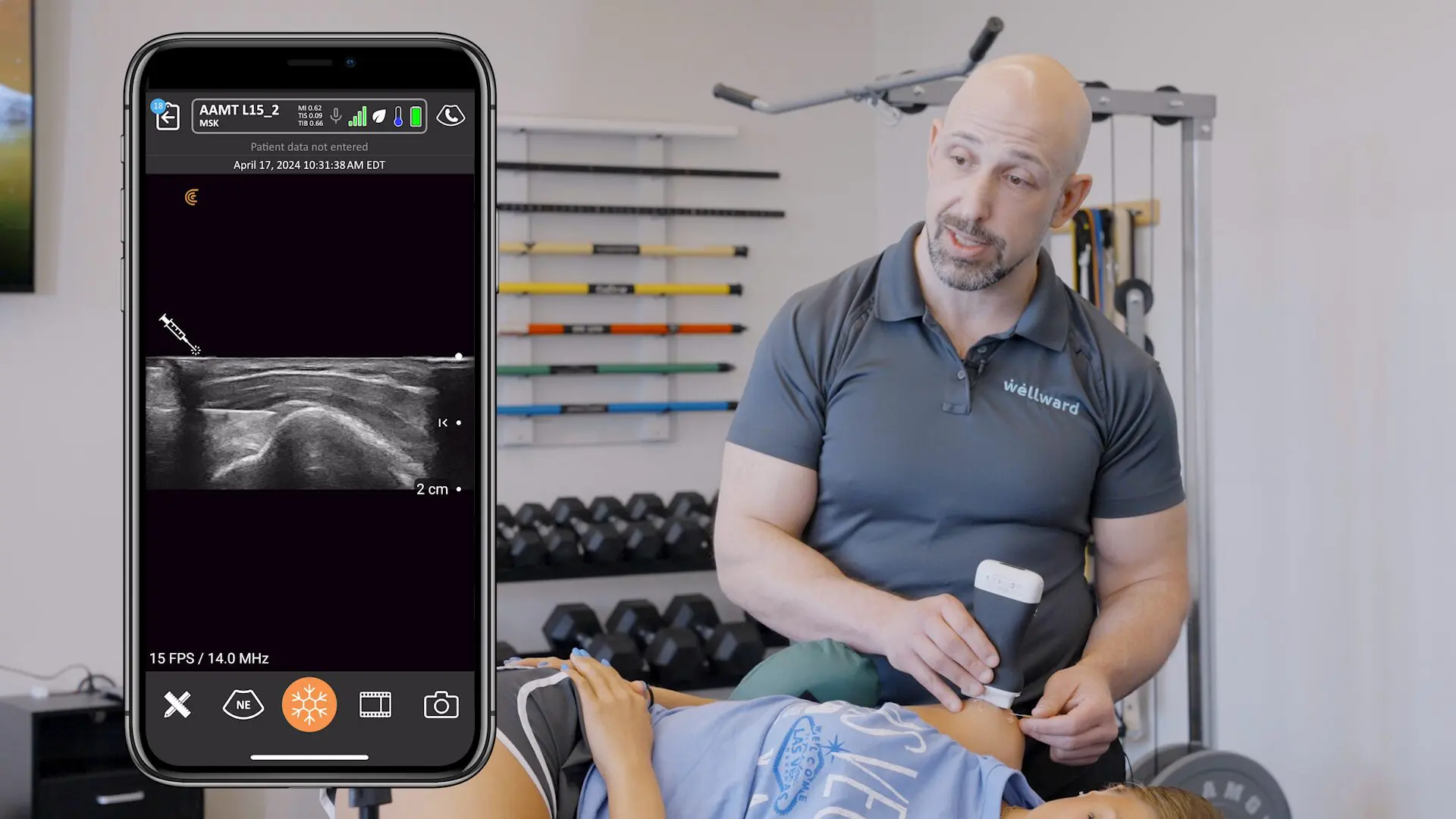
In the webinar, Dr. Hirahara demonstrates the difference between in-plane and out-of-plane injection techniques using ultrasound. His preferred technique is in-plane, which allows the best and most complete visualization of the needle. With good in-plane technique, no special reflective needles are required, and you can see exactly where you’re injecting.
Bicipital Groove and Subscapularis Injections
Dr. Hirahara stresses there is no one technique that’s perfect for every situation. From experience, he developed a technique of imaging the biceps tendon in short axis, injecting from a lateral approach, externally or internally rotating the arm for easy access to the groove. This enables complete visualization of the needle to inject either into the tendon or sheath. This approach also allows nice access to the region of the subscapularis by simply advancing the needle across lesser tuberosity.
Watch the video:
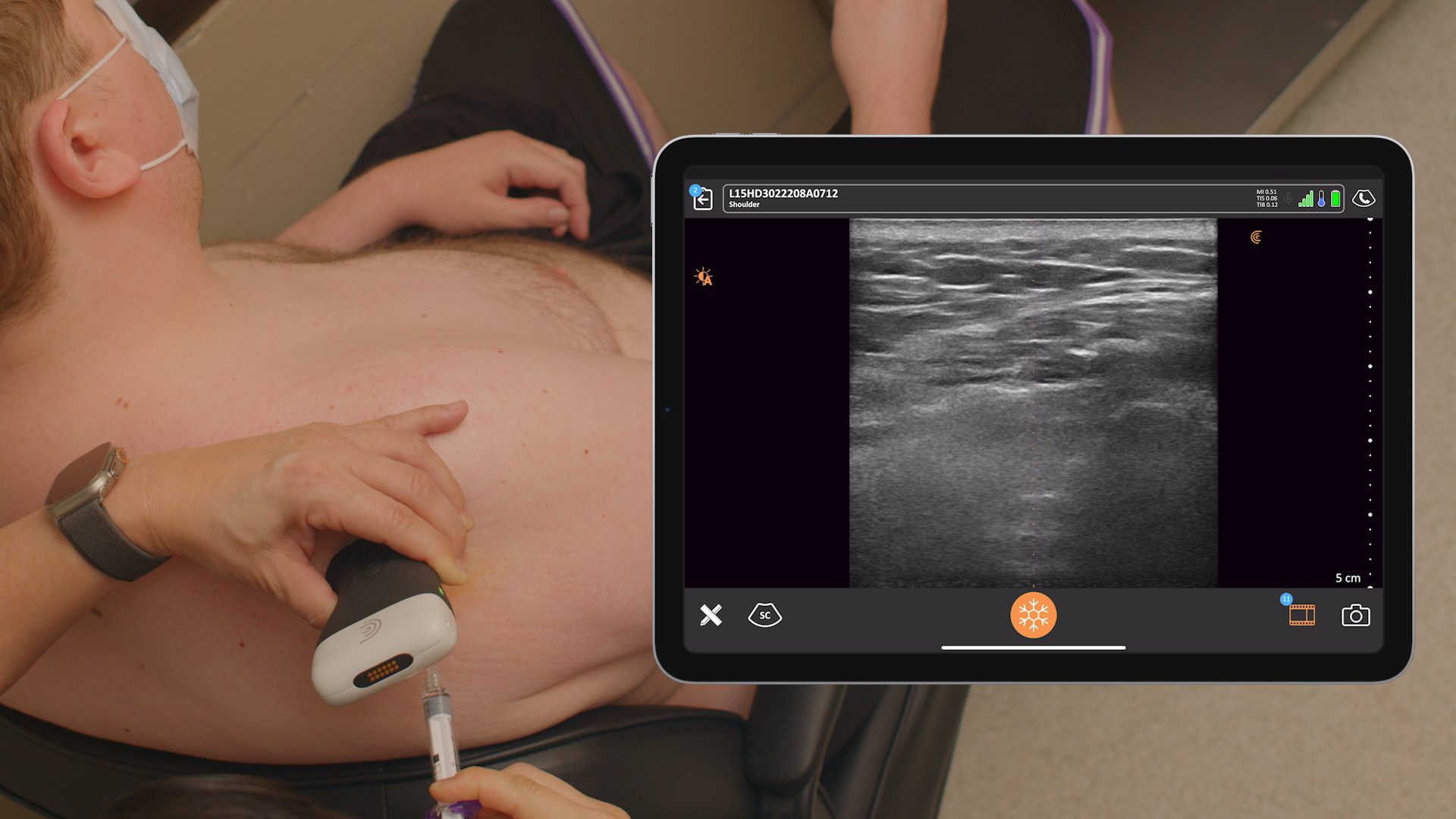
Supraspinatus and Subacromial Injections
According to an article from the Journal of Ultrasound, ultrasound-guided injections into the subacromial space are much more accurate and effective compared to those performed blindly.
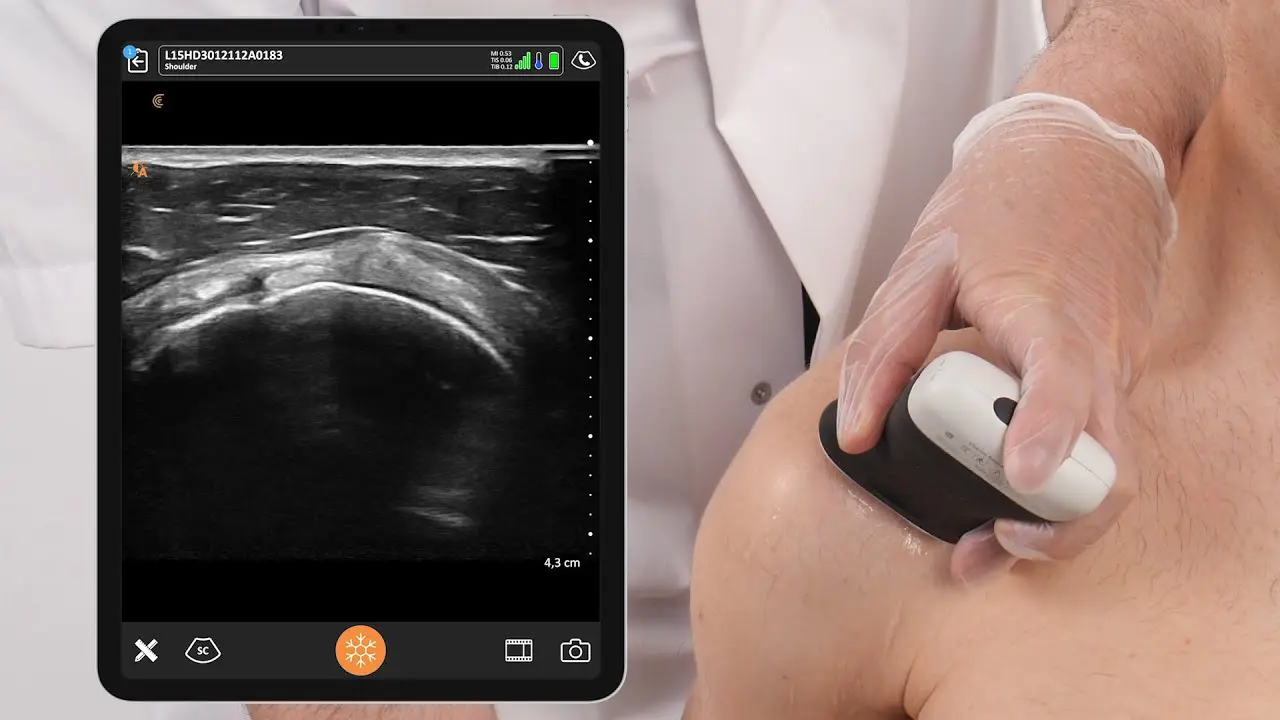
And with the injection of orthobiologics into pathologic tendons, precision matters more than ever. Dr. Hirahara positions his patients so he can image the supraspinatus in long access, and again, perform the injection in-plane to optimize the injection.
Watch the video:
Glenohumeral Joint Injections
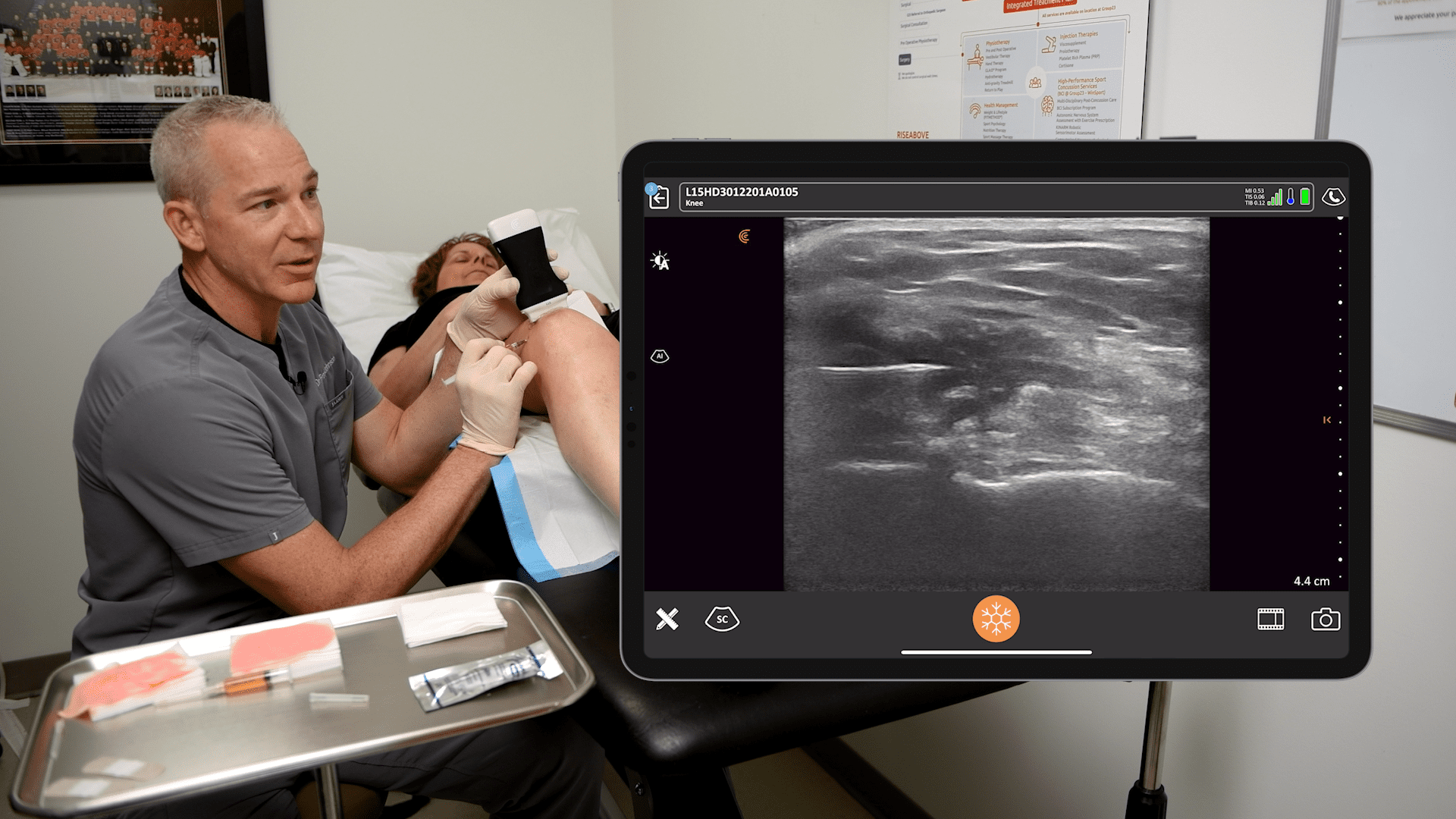
This is an injection Dr. Hirahara prefers to do out-of-plane because of the depth of the joint. In his experience, in-plane injections with a posterolateral approach are more painful and there is a risk of damaging the articular cartilage of the humeral head. It’s easy to visualize the joint. Dr. Hirahara centers it on the ultrasound screen and uses the center line marker on the image to guide the needle into the joint.
Watch the video:
AC Joint Injections
The AC joint is typically imaged in long axis, where both the acromion and the clavicle can be visualized. From this angle, an in-plane injection can be tricky, and may not get to the joint space. When the scanner is rotated 90 degrees and angled slightly toward the patient’s head, the joint space is better visualized, and a more accurate in-plane injection can be achieved.
Watch the Video:
Ultrasound Assisted Surgery
High-resolution ultrasound can be extremely helpful in surgical planning. Dr. Hirahara describes the use of ultrasound prior to biceps tenodesis. The biceps tendon is located as it exits the groove, above the pectoralis major and the skin is marked to indicate the location of the portals for arthroscopic biceps tenodesis, making the procedure safer and more accurate. Refer to his publication for more details.
Watch the video:
In summary, ultrasound:
- Is a tool like fluoroscopy or arthroscopy
- Is inexpensive and widely available
- Allows for visualization of anatomic structures
- Helps guide injections and surgeries
- Transforms surgeries from open to percutaneous
These are just a few of the ways Dr. Hirahara incorporates ultrasound into his practice. Stay tuned for upcoming webinars to learn more ultrasound tips and tricks to optimize orthopedic surgeries and injections.
Eliminate Guesswork with Clarius HD3 Ultrasound for MSK Procedures
Thanks to miniaturization and innovation, high-definition imaging with ultrasound is now easy and affordable. Clarius offers image quality that is comparable to compact ultrasound systems for a small fraction of the cost. To learn more about the high-frequency Clarius L15 HD3 handheld ultrasound scanner Dr. Hirahara uses, contact us today or request an ultrasound demo. We would love to show you the difference high-definition imaging makes for orthopedic surgery, so visit our Orthopedic Specialty Page where you can access additional Webinars, Testimonials, and Classroom Videos.