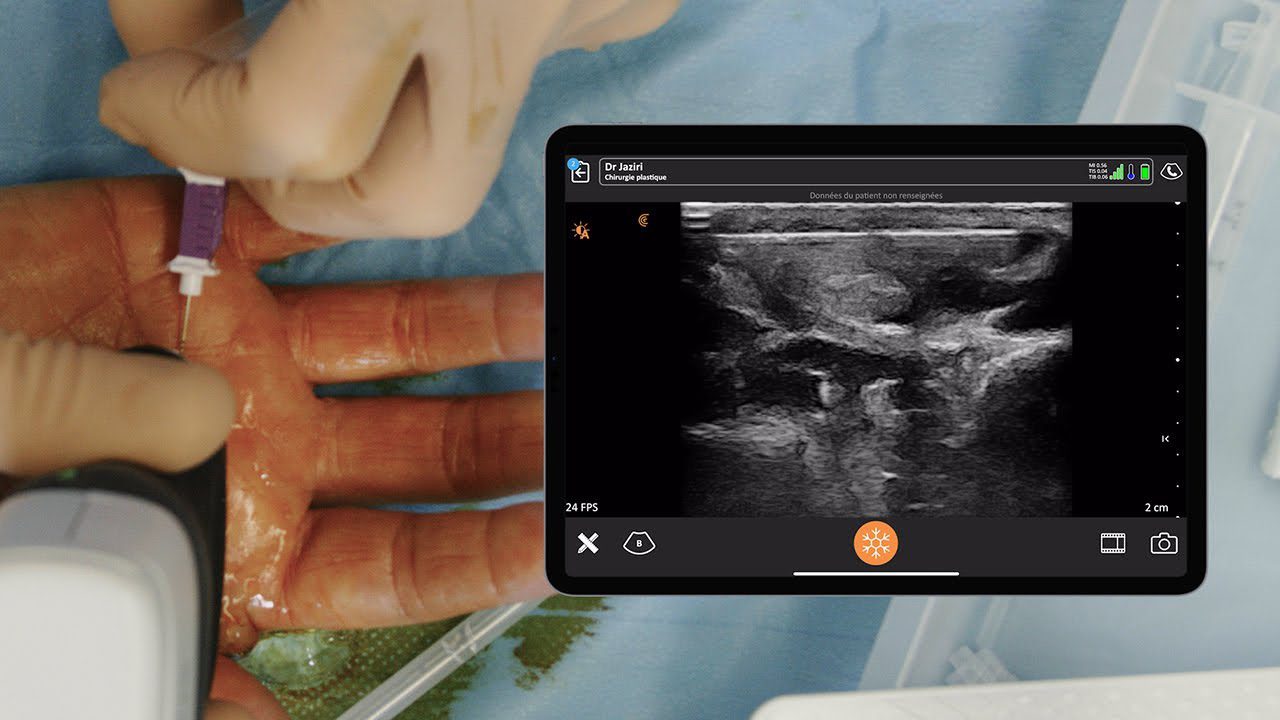
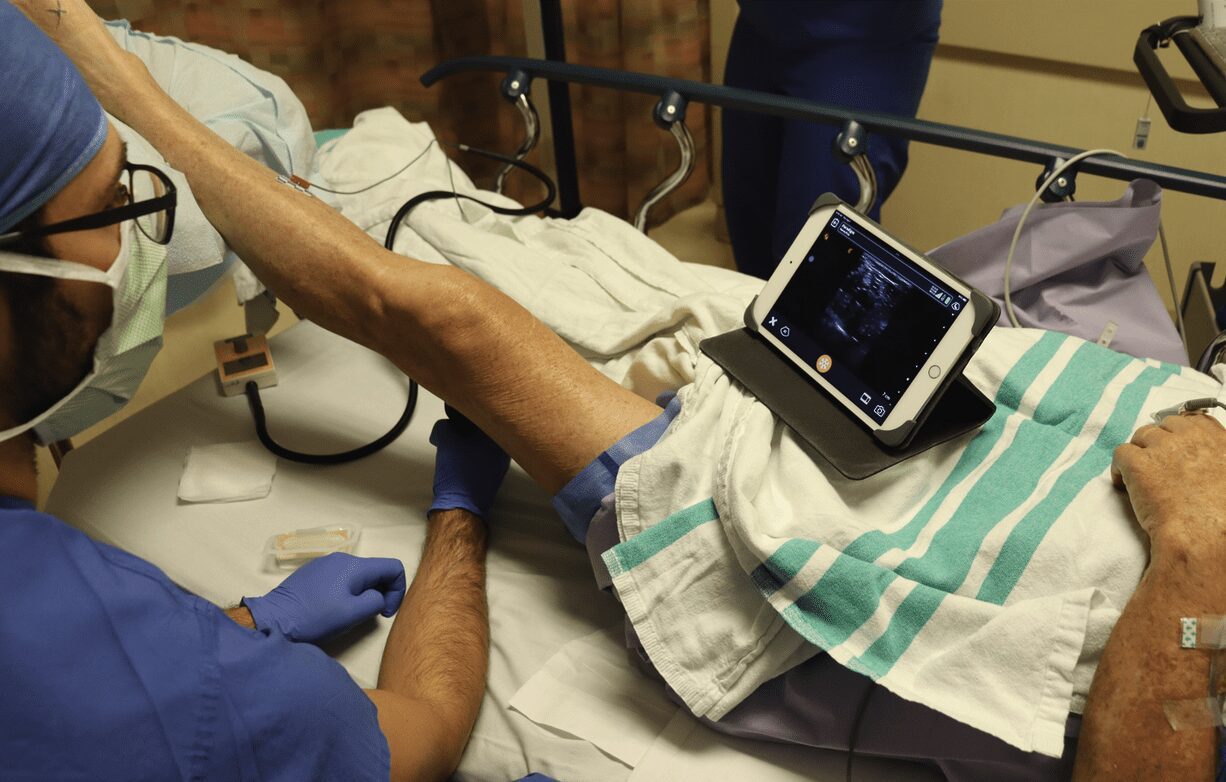
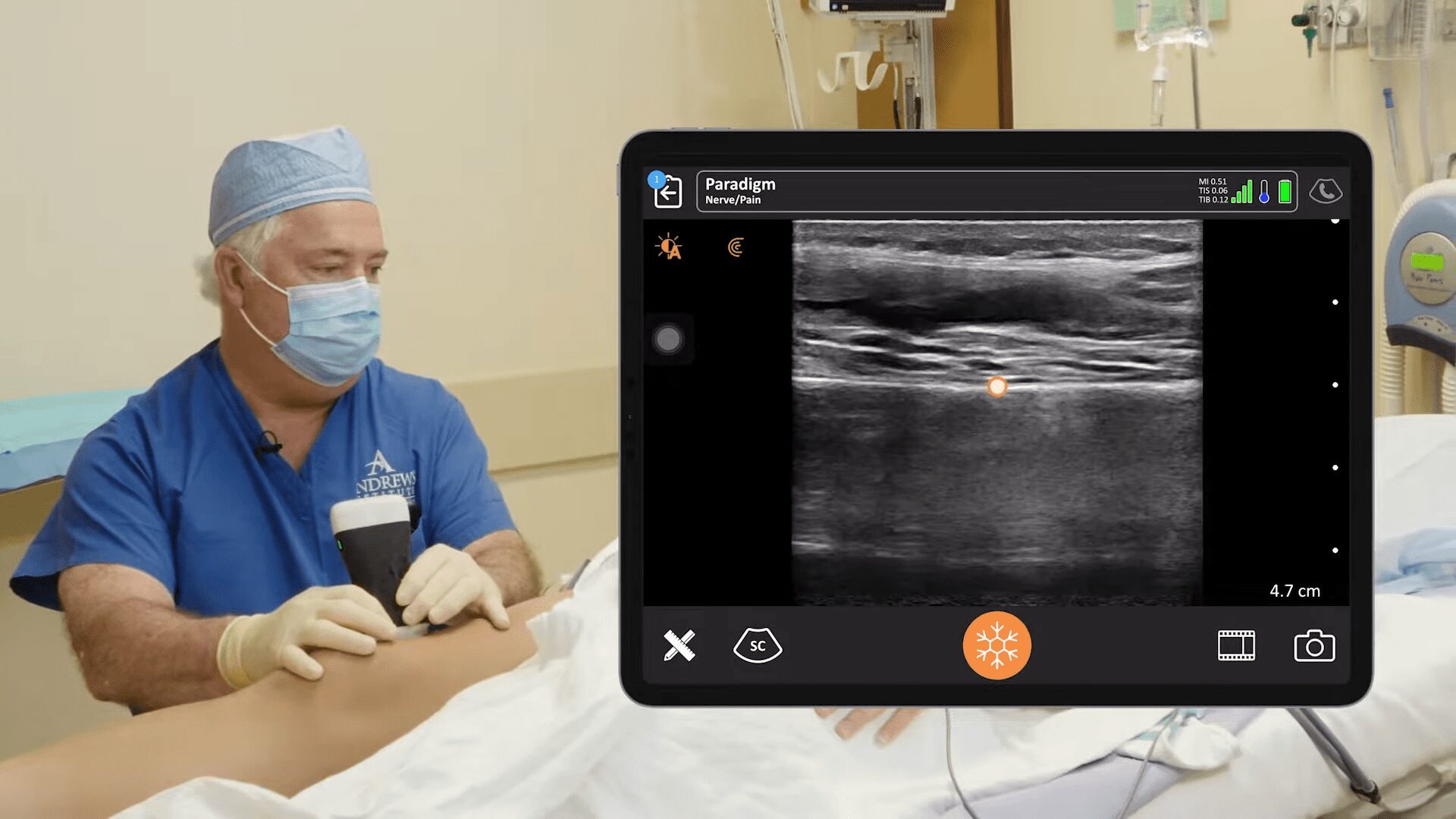
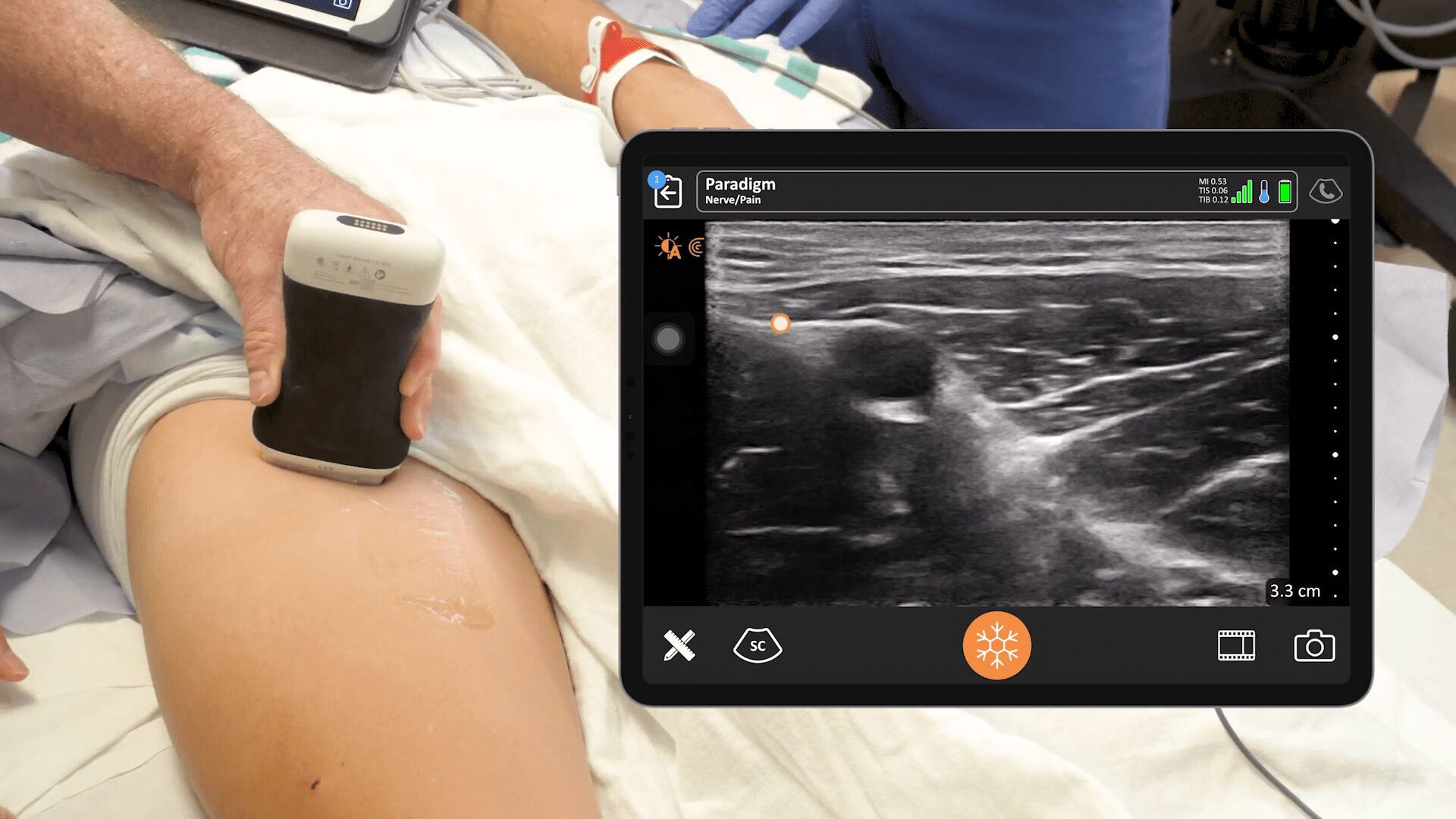
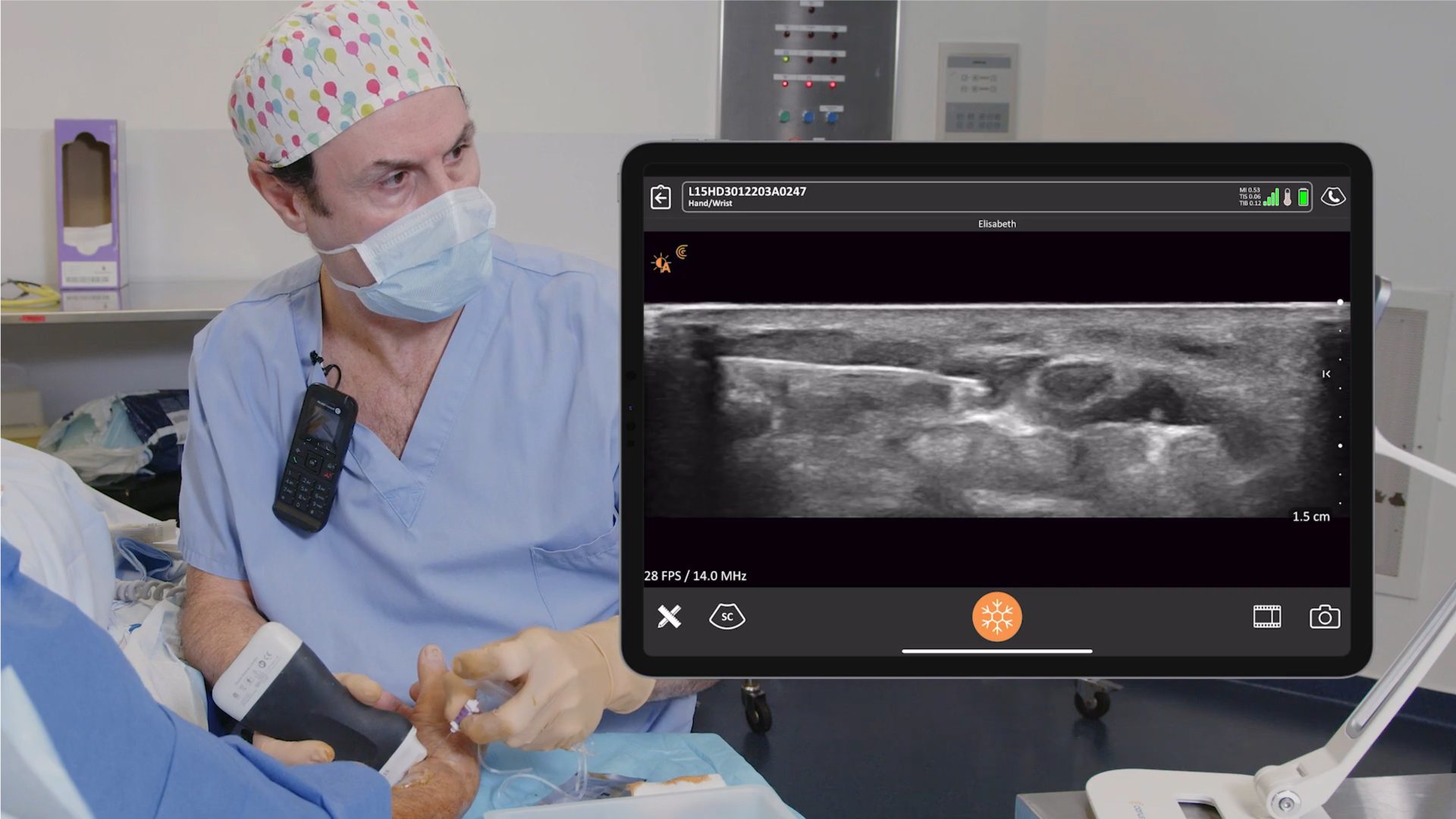
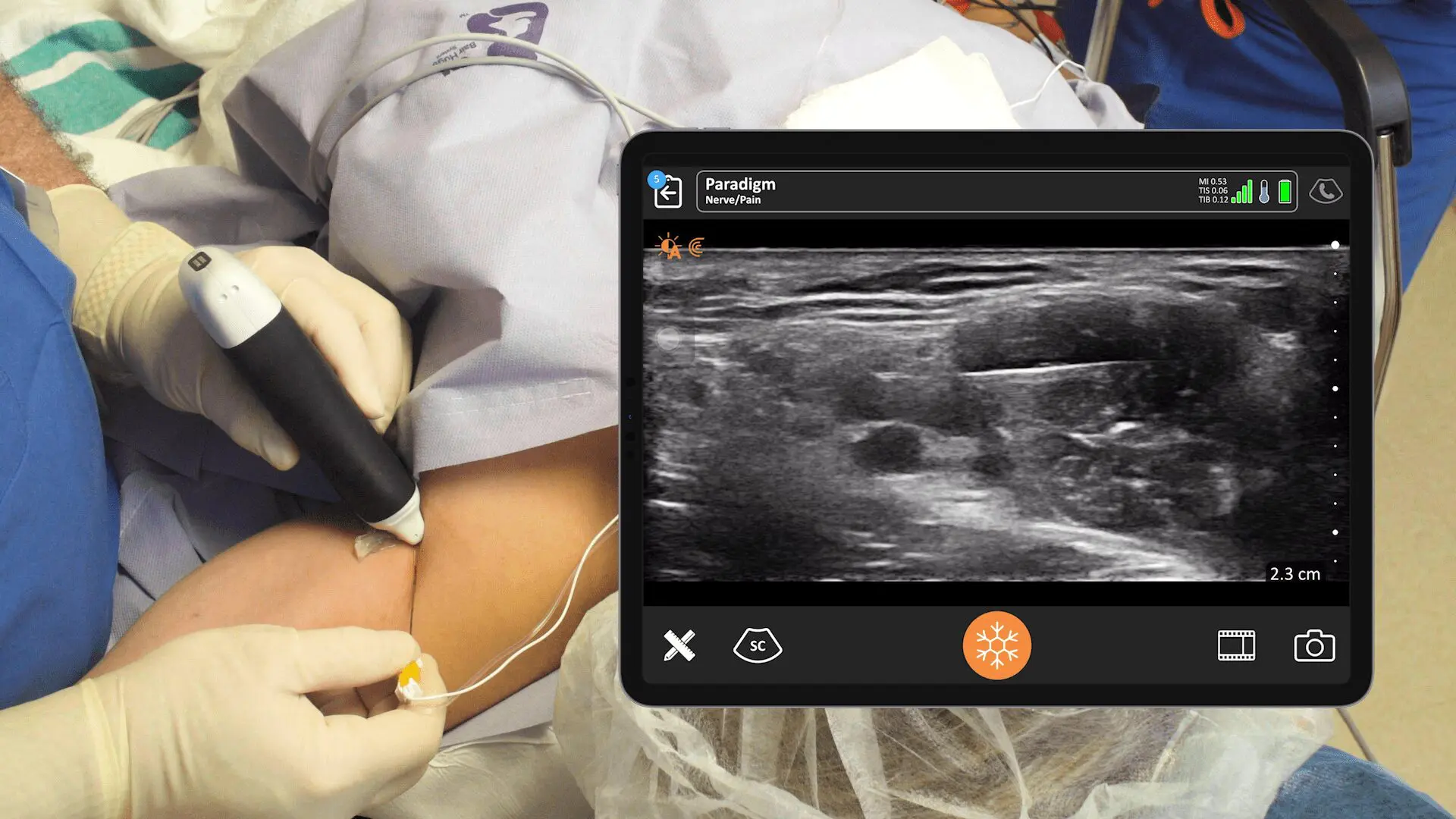
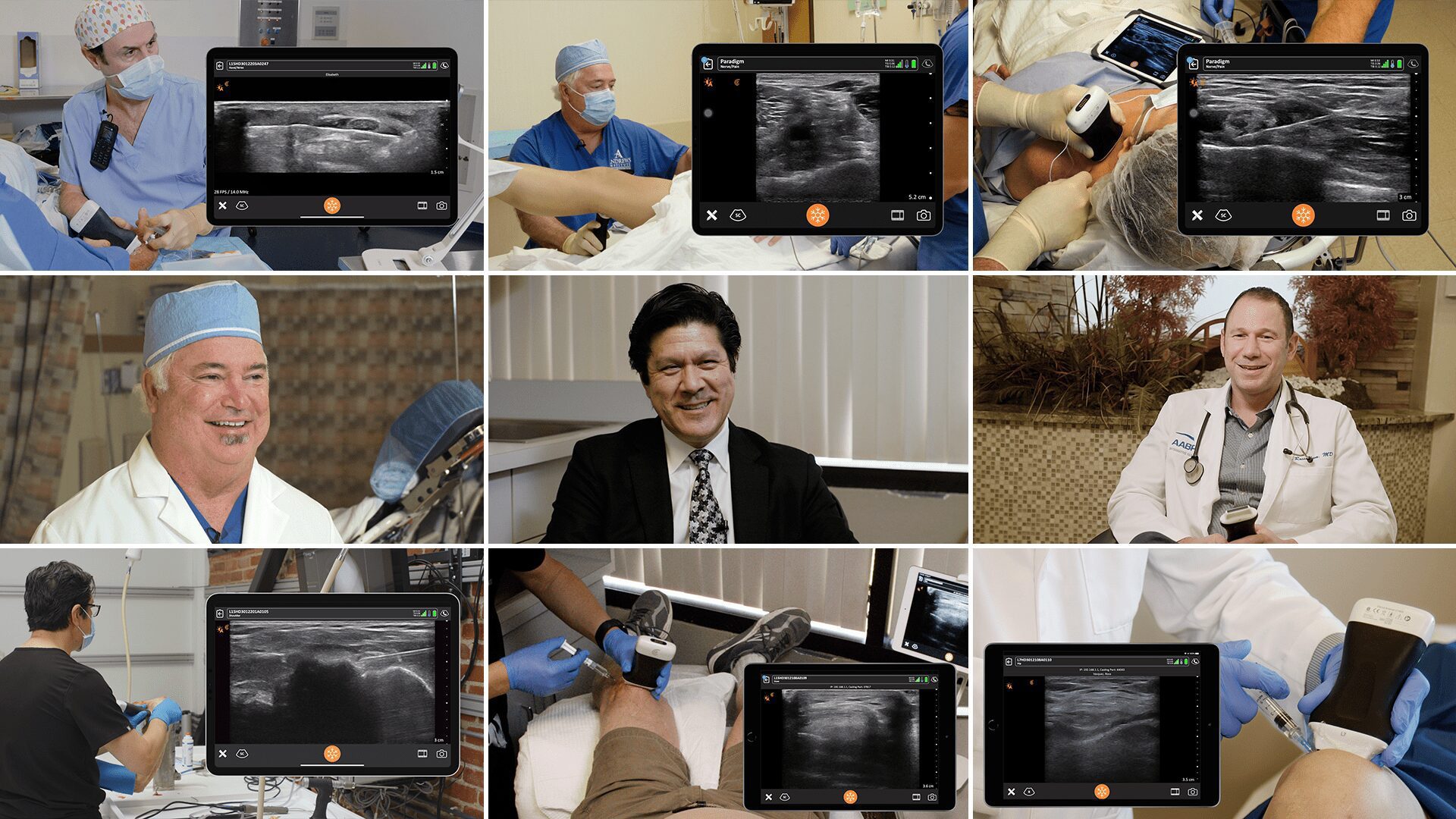
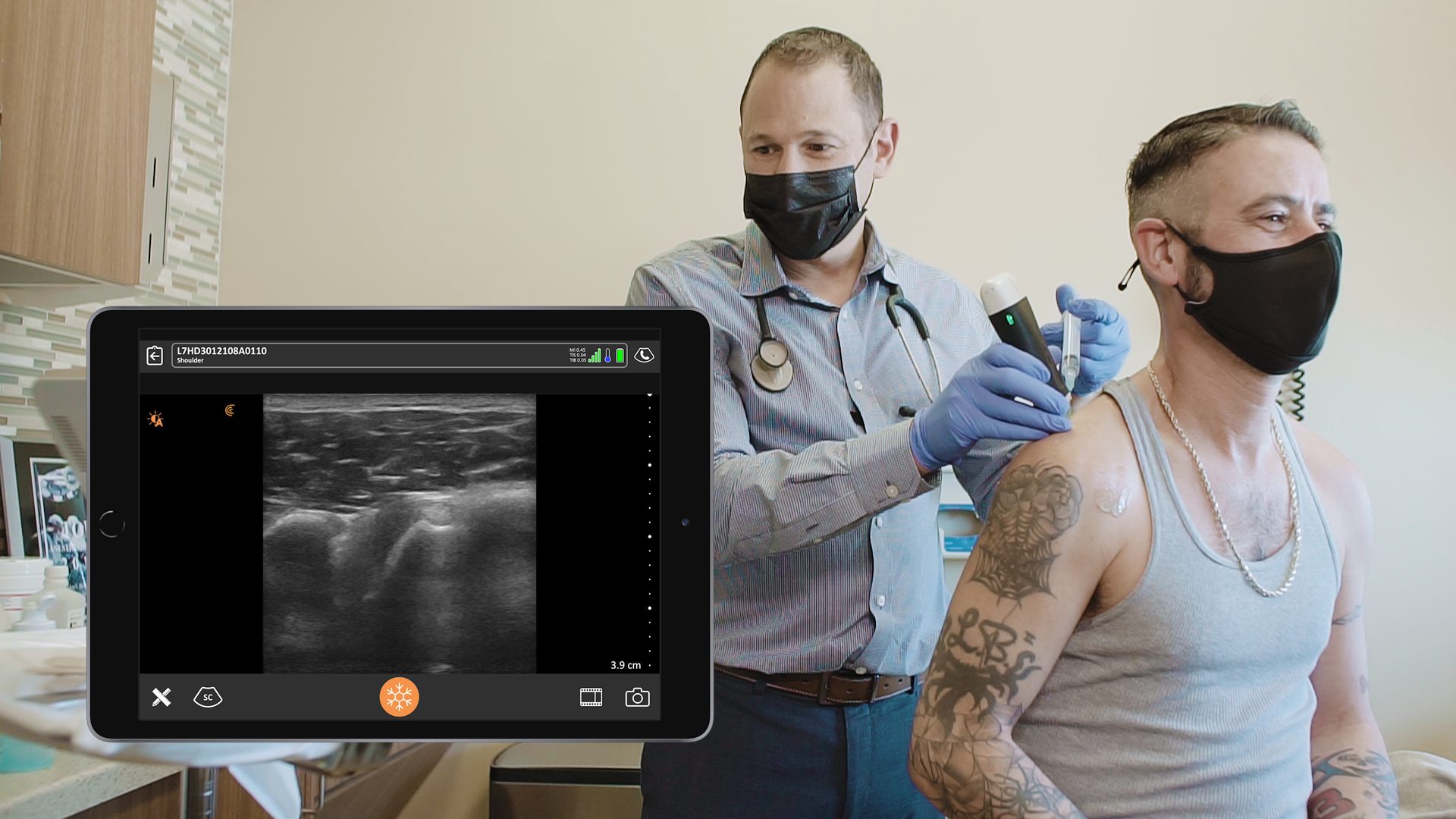
Dr. Oron Frenkel is a practicing emergency physician, passionate POCUS educator and serves as chairman of the Clarius Medical Advisory Board. He recently moderated a webinar featuring Dr. Greg Hickman and performed a literature review as part of his preparation. Following are his findings.
We all know that ultrasound has been used for guiding regional anesthesia for almost 25 years and it’s no surprise it has gained enormous popularity in the past decade. Every five years, as more and more research is published, ultrasound use seems to be exploding both with the techniques available and the applications. It’s basically common in daily practice and the number of practitioners using it worldwide is increasing day by day.
ASRA Review Confirms Benefits of Ultrasound Guidance for Regional Anesthesia

In my literature review, the best data we have I think, comes from the ASRA reviews and they’ve done two now. The most recent one was published in 2016. ASRA assembled an expert panel to systematically review the field studies. The expert panel found a couple of really interesting findings in their last publication.
First, it backed up the finding that ultrasound is rapidly becoming the default nerve localization technique. It’s really the standard way that clinicians are learning to find the nerves in the body and to identify them, especially for novices and trainees during their educational period.
Next, and what’s more interesting, is the findings that the use of ultrasound has on the sensory and motor block. It decreases the performance time, the time to produce and get your block into the patient, and it results in fewer needle passes because we’re visualizing the needle. All of these translate into obvious clinical benefits for the anesthesiologist and the patient.
Use of Ultrasound Reduces the Risk of LAST

When we dig a little deeper, it’s quite definitive that the use of ultrasound significantly reduces the risk of LAST (local anesthetic systemic toxicity) which is, of course, the most feared complication of regional anesthesia. Even though LAST sometimes occurs with ultrasound-guided procedures, the significant reduction in its incidence starts to prove that ultrasound really is improving clinical care.
Another interesting finding, especially with upper extremity blocks, is that the incidence and intensity of hemi diaphragmatic paralysis is reduced with ultrasound guidance. This is likely the result of being able to use smaller amounts of medicine and lower doses because it’s more targeted injections.
The ASRA paper stops short of calling ultrasound guidance for regional anesthesia standard of care. One of the issues pointed out was the lack of available ultrasound machines at all locations, which limits widespread use, which is a fair point.
Emergence of Handheld Ultrasound is Making Ultrasound Guidance More Accessible

Now, five years after this review was last published, we now have handheld ultrasound systems. This new generation of point-of-care ultrasound devices makes ultrasound guidance much more accessible to practitioners everywhere.
Yes, at present, there is little uniform teaching of ultrasound skills to anesthesia residents, faculty and staff members. Not everyone has an instructor knowledgeable in point-of-care ultrasound or bedside ultrasound with them whenever an ultrasound examination or a procedure is warranted.
Although we think that handheld ultrasound really can set the standard in the coming years, we know that we have to focus on better training. That’s why I’m happy to collaborate with Clarius and ultrasound experts from various medical specialties to present training in the form of webinars and video tutorials that are broadly available.
Learn Master Tips for Using Ultrasound for Regional Anesthesia
I recently had the pleasure of hosting the webinar “The Mobile RA – Using Handheld Ultrasound to Guide PEC and Supraclavicular Blocks Plus Intra-Articular Injections” with Dr. Greg Hickman who has perfected the art and science of ultrasound-guided injections to deliver maximum pain relief. Dr. Hickman is the medical director and anesthesia director at the Andrews Institute Ambulatory Surgery Center in Gulf Breeze, Florida. He is also co-founder of the popular ultrasound-guided regional anesthesia education website, blockjocks.com, which teaches doctors, nurses and patients around the world.
We invite you to watch a recording of the webinar to learn his master tips to guide PEC and supraclavicular blocks and intra-articular injections using ultrasound.”
Interested in Using Clarius Ultrasound for Your Regional Anesthesia Practice?
Wireless and pocket-sized, Clarius scanners deliver the high-definition imaging and power you expect from a traditional ultrasound system in a highly affordable ultra-mobile scanner. Visit our regional anesthesia specialty page to learn more about Clarius. Or book a demo for information on which Clarius system is right for you.