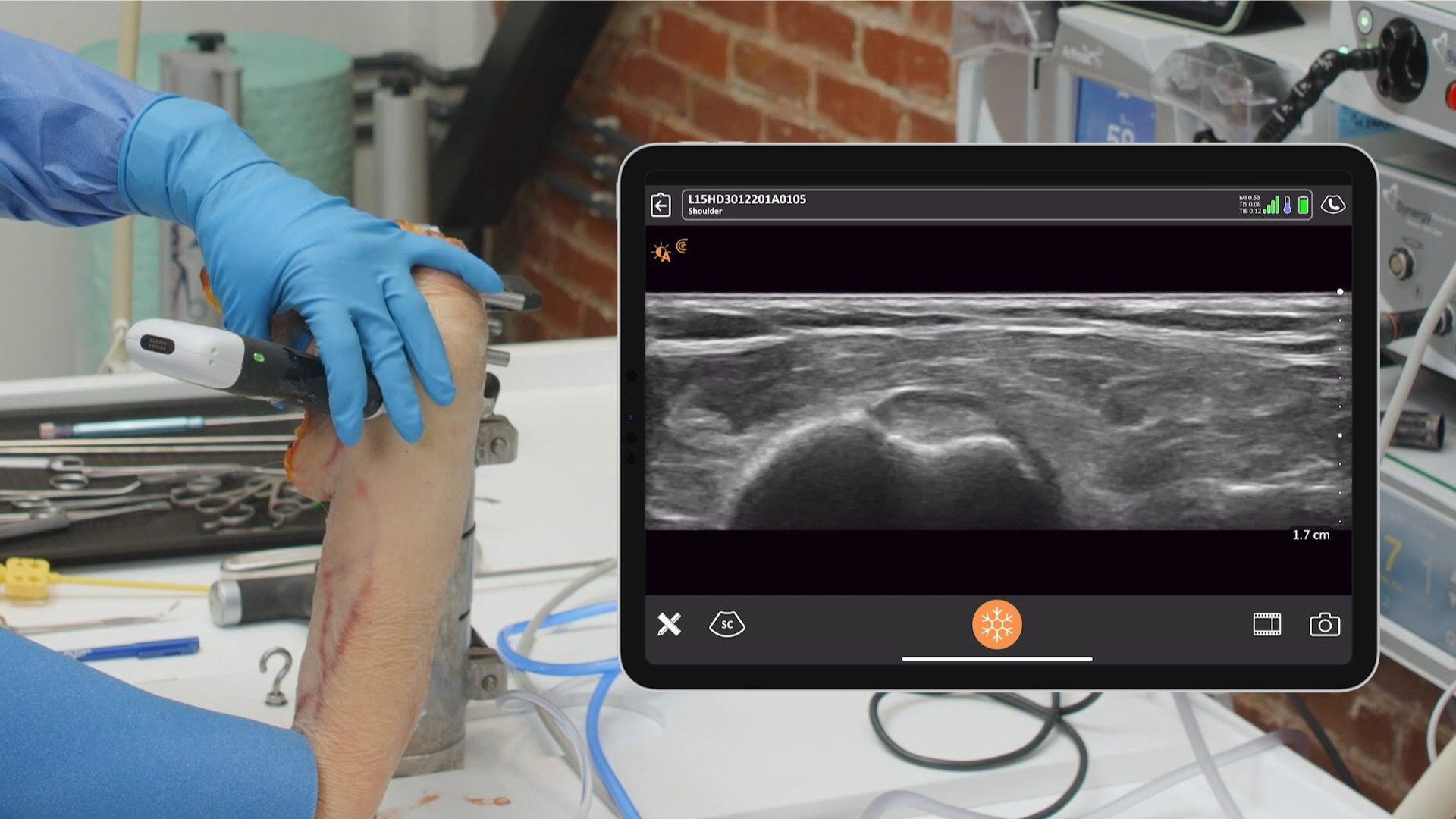
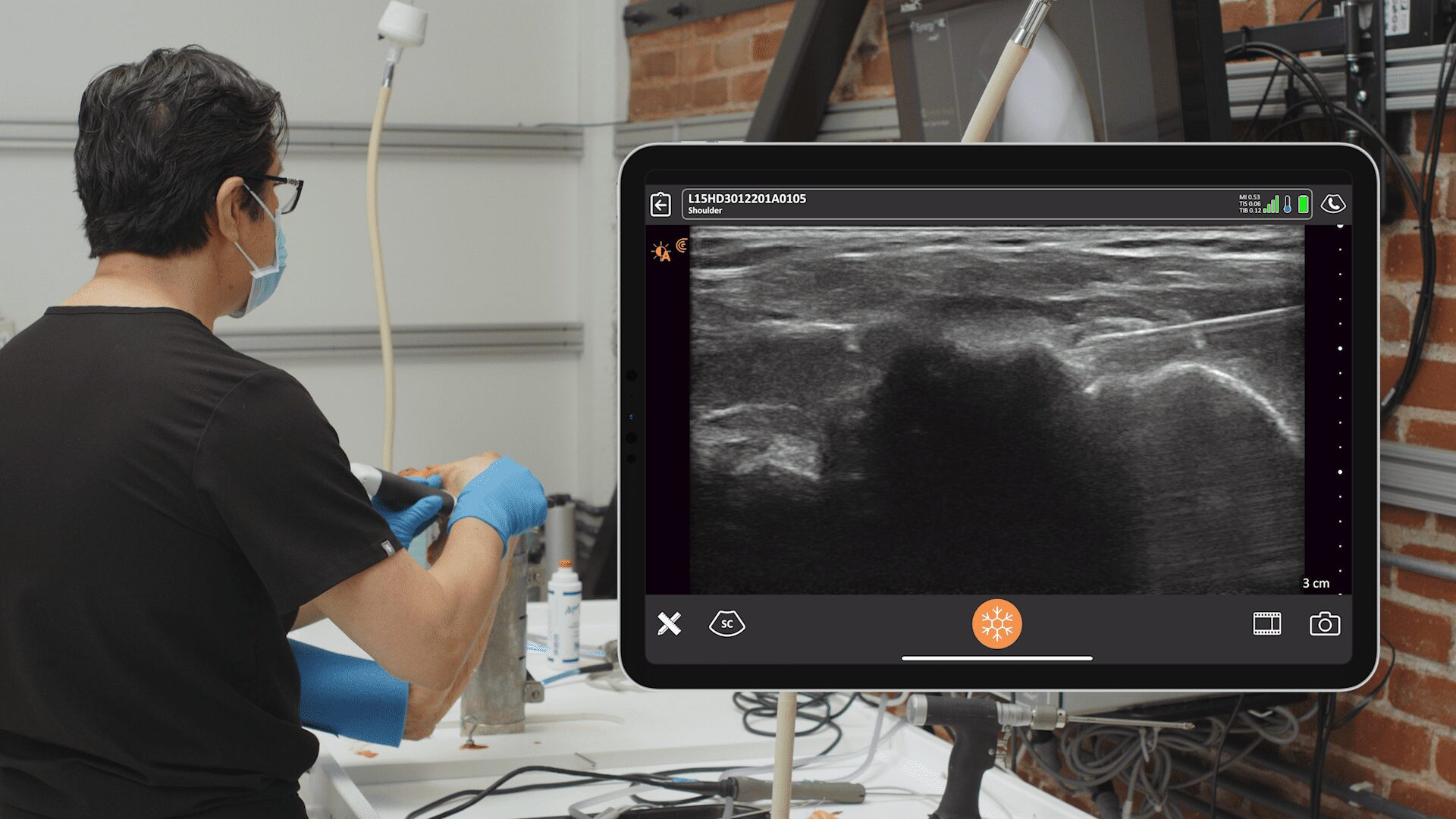
Dr. Alan Hirahara is an orthopaedic surgeon who has been in private practice in Sacramento, California for 20 years. He is an expert in orthobiologics and has been a team physician for Sacramento State and the Sacramento River Cats (Triple-A affiliate to the San Francisco Giants). A trailblazer amongst his peers in the United States, Dr. Hirahara has been using ultrasound for more than a decade at his clinic and in surgery. We recently had an opportunity to speak to him about his experience with Clarius ultrasound and why he believes ultrasound will become the standard of care for orthopaedic medicine. Here’s what he had to say.
What inspired you to start using ultrasound in your practice?
“I started using ultrasound in 2009. I had just come back from a meeting on orthobiologics in Munich, Germany. I realized at the time that the Europeans and the Asians were absolutely outstripping us in their usage of orthobiologics. And the reason they could is that they actually didn’t have as much access to MRI’s, and they had to use ultrasound. It turns out that it was actually a boon for them and something that we needed to do. While you can’t bring a needle into an MRI machine, you can use ultrasound to guide a needle to precisely place your biologics into specific pathologies. So, I came back and within three weeks had a machine in my hands and getting very dangerous with it. It was incredible. It opened my eyes completely.”
Why do you think more of your peers should be using Ultrasound?
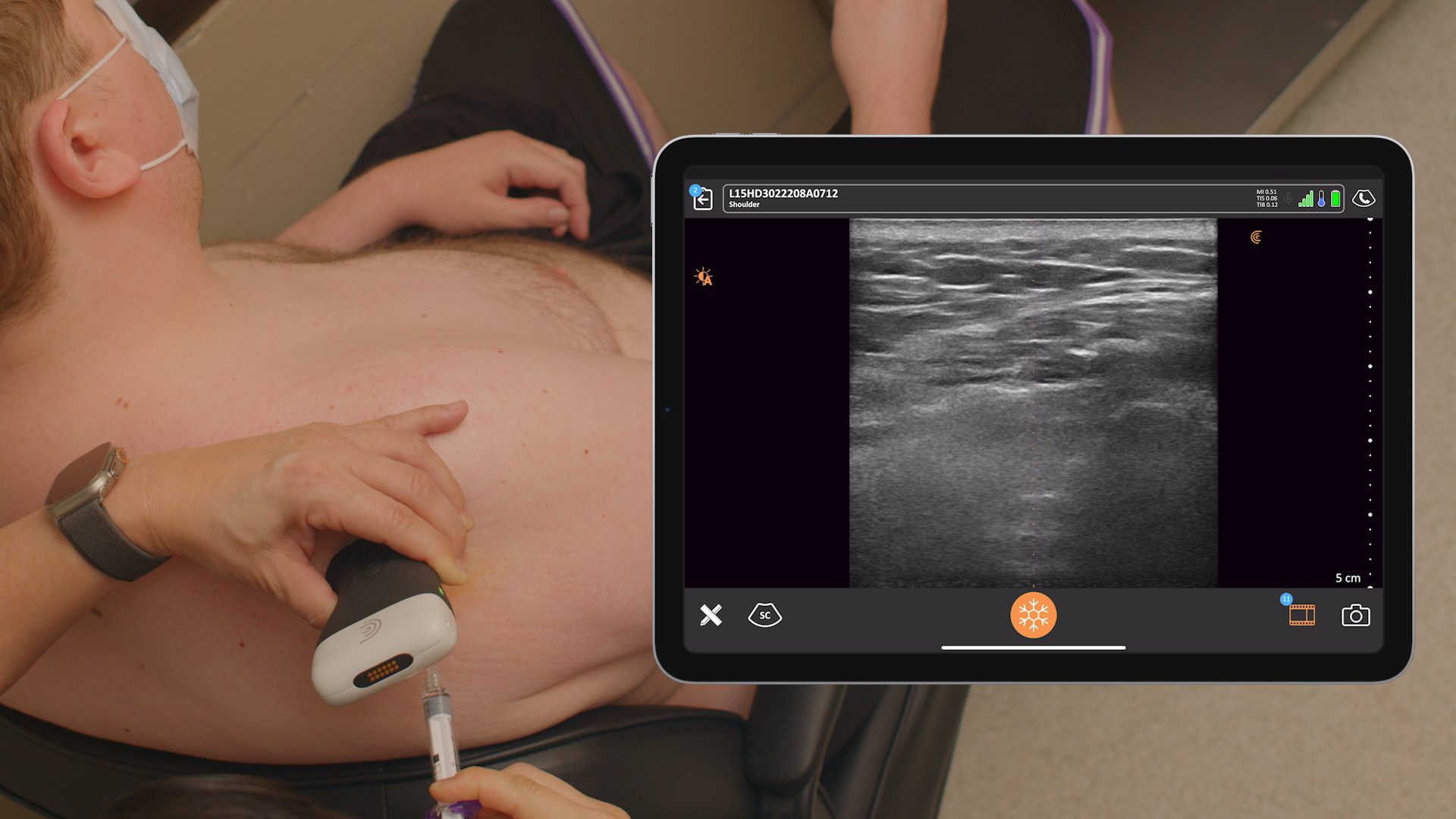
“When you inject into the right spot, your patient doesn’t feel pain. When I first started practicing, I thought I was really, really, really good. But it turns out I wasn’t. And the reason was that if you’re placing an injection into a joint or a space, like the subacromial space, there shouldn’t be any pain because it’s open space. There’s no nerves so you shouldn’t feel it. And so why should all these injections be so painful? Well, the obvious answer is: I was missing. And it turned out once I started using ultrasound it could be point specific. None of my patients had pain unless I put it into a structure that I wanted to go into intentionally, like a tendon, ligament, or muscle.”
Do you see ultrasound adoption becoming more widespread?
“I think surgeons are biased and they think that they can do things blindly because that’s the way they were trained, and because they think they know where things are and how to get there. It turns out you just don’t. And what surprises me is that we use fluoroscopy and arthroscopy a lot. So why wouldn’t ultrasound, yet another tool in our hands, be just as useful and good? And it is.
What’s great is it is coming. I’m seeing a change in the training, in residencies, in fellowships, and people coming out. The newer generations are absolutely being acquainted with it, taught it, and it will eventually become the standard of care, which it should be.”
What are the downsides of relying on landmarks for procedures?
“You’re going to hurt your patients. And the reality is, you’re not going to do a good job. If you place cortisone into a structure like a tendon or a muscle or a ligament or fat, you get necrosis: it damages the tissue. It’s not good for the tissue. Even going peri-structure is not ideal, but still acceptable. So going into a structure is going to do harm to it.
If you’re going to do orthobiologics, which are not necessarily covered on insurances, you want to make sure your patients get the most from their money. You better get it in the right spot for the right reason. It’s all the more reason you need to do ultrasound. It’s been proven over and over again. There’s plenty of studies at this point that have absolutely proven the validity and reliability of ultrasound guidance as the best way to make sure you are in the right spot.”
Do you have suggestions for someone who is starting to use ultrasound for orthopedic medicine?
“When someone’s first starting out and they want to get into ultrasound, I actually think the Clarius handheld ultrasound system is an ideal first step. And the reason why I think so is it’s so well priced and gives you such good quality. It’s an ideal situation for someone to try it out and not take a huge loss. And frankly, with the reimbursement that we get today with ultrasound guidance and usage on the codes, you’re going to easily make that money back, no problem.”
When do you use Clarius ultrasound?
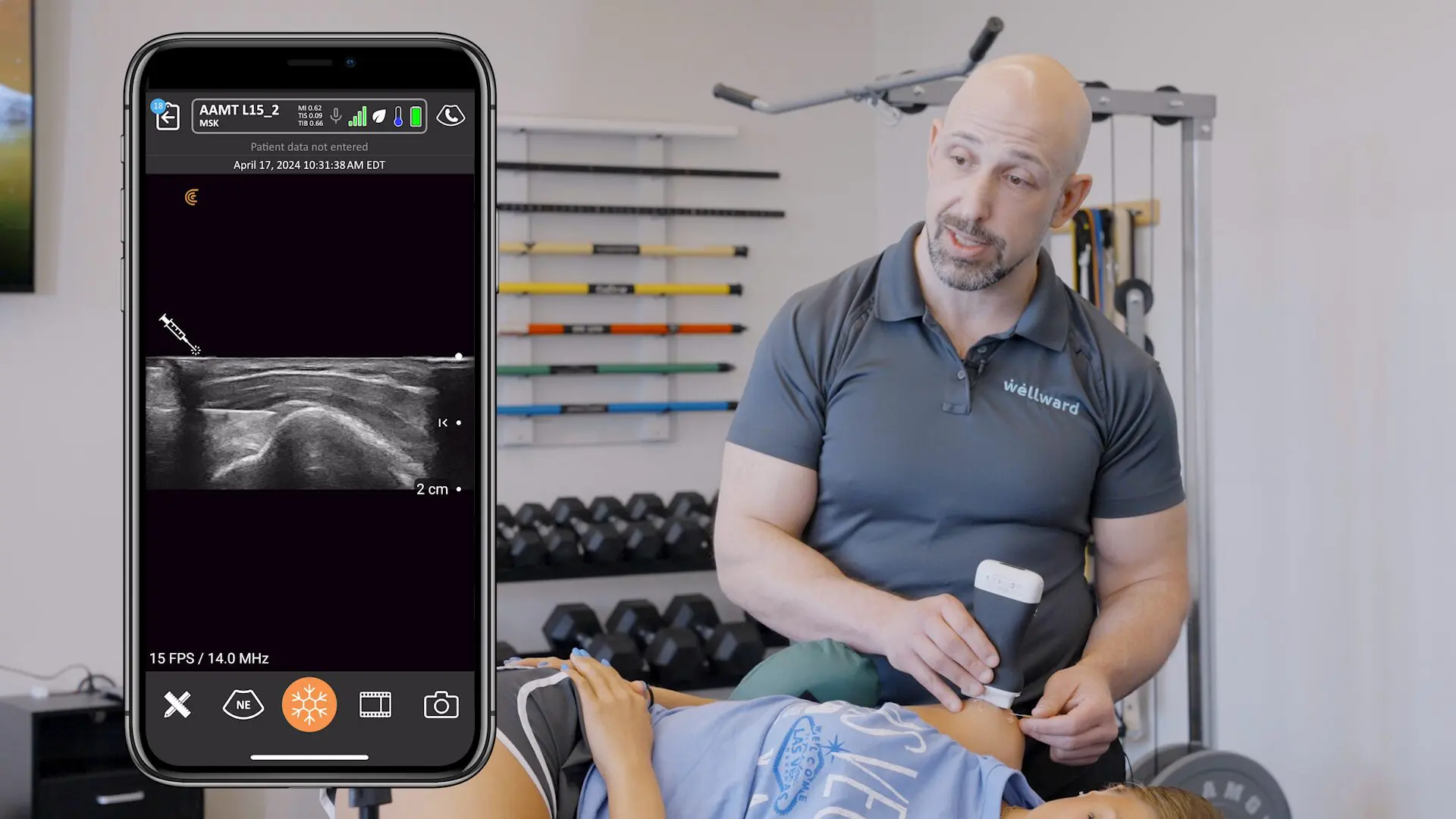
“For me, I use it as my accessory. I use the larger systems for some of my in-office clinic finer detail work, but this system is absolutely ideal for the accessory unit I need in my clinic to run a second or third room with my fellows in-office. I also take it with me on my trips when I have to go to courses I teach, or if I have tocover a game and have that unit on the sidelines.”
What do you like about Clarius HD?
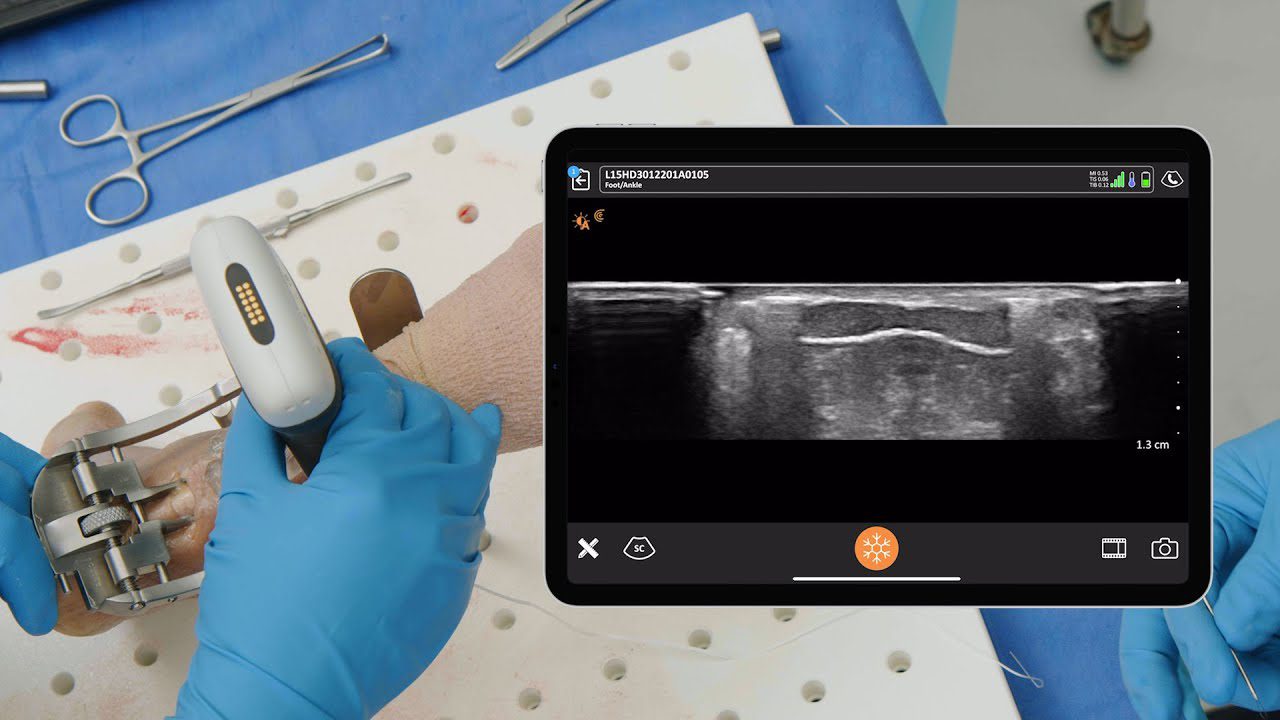
“For me, being able to bring it into the operating room and pop it into a bag that’s sterile is so much better than having a cord that could be prone to contaminating the surgical field. And you have to have that monitor so close to you because you’re tethered by a cord. Now, you can be wireless and be as far from it as you want. I can be on a big screen, because it doesn’t matter what kind of screen you use. And then of course, as a sports specialist, covering events and games being on-field, that’s literally the definition of point-of-care. I can be there on the field, pull it out of my pocket, and just use my phone or my iPad to do a quick scan on someone instantly. That is outstanding. I really wasn’t aware that this was going to be such an important device for me.”
What do you think about the quality of the images you get with Clarius?
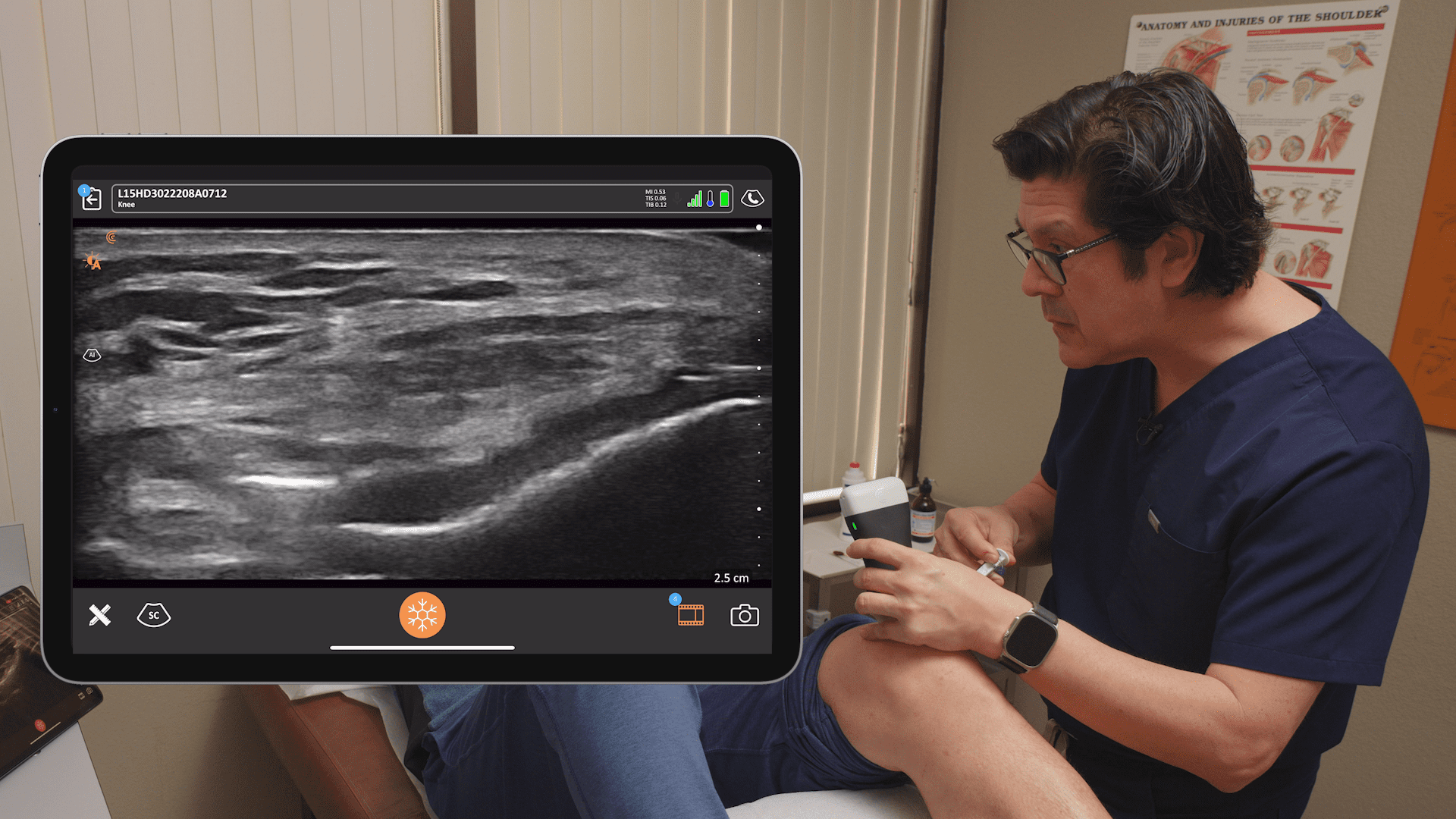
“At this price point, the Clarius image is very, very high quality, high class. It’s amazing that you get such a great image on a wireless system and in such a small handheld system. Is it as fine as, say, a hundred or $200,000 machine? Well of course not, but that’s no surprise. But for the value you’re paying, for what you’re getting, and for its usage, it’s amazing. For me, it can diagnose easily big structure problems. You can diagnose some of the subtle, small, partial tears of cuff or things like that. Sometimes you can see them, sometimes you can’t, but even on the bigger system, sometimes you can’t tell either. The reality is, it is absolutely on par with what I expect and better. For the quality and the value you receive, it’s amazing.”
Have you tried other handheld systems? And if so, how does Clarius compare?
“I have used other systems, and this absolutely compares highly favorably. The image quality in my opinion is higher. Yes, in some instances, this unit is more expensive, but to me if you compare the quality and the value you’re getting, you’re paying for the high quality image. That value is incredible. It’s worth the extra small amount of money you’re paying compared to some of the other handhelds that are marketed out there today. To me, it’s absolutely worth the value. And every time I show it to someone to compare, there’s no doubt it excels and beats the others.”
Learn from an Ultrasound Master: Register for a Free Webinar with Dr. Hirahara
We invite you to register for a one-hour webinar with Dr. Hirahara on October 12: Visualize Your Needle: Ultrasound for Painless and Accurate MSK Injections.
In this 1-hour webinar, you’ll learn how effective, easy and affordable it is to add handheld ultrasound to your practice. Dr. Hirahara will teach:
- Basics on POCUS-guided treatment modalities for MSK pathologies
- How to perform painless and slick ultrasound-guided knee injections
- How to accurately inject into the subacromial bursa rather than near it
- How to use ultrasound to guide tendon injections for maximal benefit
For more information on Clarius ultrasound for orthopedic surgery, visit our specialty page or contact us for a live demonstration.